
This is an update of previous story published on July 14, 2020.
In early spring, health officials and providers across California braced for a flood of coronavirus patients. Spread of the disease elsewhere—such as New York, with hospitals and morgues overwhelmed—led epidemiologists to forecast a surge in the Golden State by mid-April.
That surge did not materialize. Orders issued by Gov. Gavin Newsom requiring residents to stay at home as well as restricting public gatherings and non-essential businesses—combined with initial adherence to public health department guidelines on social distancing, hand washing and face coverings—seemed to work for many parts of California, especially in semi-isolated rural Butte County.
In fact, among health service areas tracked nationally, the Chico area had the lowest incidence of coronavirus heading into May. In response, that month, Butte County was one of the first two counties that the governor authorized to reopen earlier than mandated for the rest of the state. A federal medical station set up at Enloe Rehabilitation Center was packed up and shipped out.
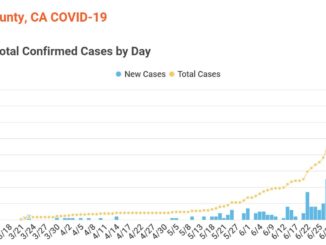
As businesses reopened, testing increased and many citizens eschewed face-covering recommendations, local coravirus began to rise sharply. As of Aug. 3, the county’s Public Health Department had recorded 980 positive tests for COVID-19, with 766 coming in July alone. Seven patients had died.
The largest spike came during the week of July 14-20, with 264 new cases, prompting the California Department of Public Health to place Butte County on the state’s County Monitoring List. That decision July 22, effective July 25, reinstituted earlier restrictions—on establishments such as gyms, hair salons and places of worship—until further notice from the state public health officer. Additionally, the Butte County Office of Education announced that, until the county has been off the monitoring list for two weeks, local schools will not open for in-person instruction.
Even with these recent developments, and with the federal field hospital no longer in place, local health administrators have expressed confidence in the county system’s capacity to treat coronavirus patients. They cite hospitals’ ability to expand intensive care should the need arise; so far, facilities have not been overwhelmed.
Butte County Public Health Director Danette York said last week by phone that she’d anticipate hospitals and clinics to experience an impact from July’s jump in positive cases over the next few weeks. Based on state and national trends, a lag (in hospitalizations, including intensive care, and deaths) tends to trail the initial wave before rising once again
“It [the coronavirus spike] has affected the health care system [already],” York added, “but not put us at a surge level.”
Enloe Medical Center CEO Mike Wiltermood concurred. Including patients from outside Butte County—Enloe draws from a service area including Glenn, Tehama and Plumas counties—the hospital has been treating between 20 and 25 a day for COVID-19, though only five to seven of those require intensive care with ventilators.
“I think we’re going to be fine,” he said by phone last week. “We’re all worried about COVID being around during the flu season, but that’s not for a few months, and we’re all keeping our fingers crossed on the progress of the development of a vaccine.”
When the governor issued his initial orders, the county’s three hospitals—Enloe, Oroville Hospital and Orchard Hospital in Gridley—joined others in preparing for surge conditions. They stopped performing elective procedures (i.e., surgeries not critical for life-saving) and dedicated areas to isolate patients. The state government dispatched federal medical stations regionally to accommodate any overflow.
The federal medical station in Chico opened in April and increased the county’s capacity for coronavirus patients by 125 beds, an additional 25 percent. Enloe, which can accommodate roughly 300 patients, was around half-full during this period, Wiltermood said. (Oroville Hospital and Orchard Hospital did not respond to interview requests.)
Unexpectedly, emergency room traffic decreased. Judy Cline, Enloe’s director of the emergency department and trauma services, said her doctors and fellow nurses consistently saw far fewer people for the illnesses and accidents that normally require E.R. visits.
“It was frightening, because people seek care,” Cline said. “Where were they? Where were they going? What was happening to them? It was very distressing for us.”
At the time, doctors still admitted very ill non-coronavirus patients to the hospital, with ample rooms available; but the volume of walk-ins visiting Enloe’s E.R. dropped from an average of 235 to 135 a day. Only in June did the E.R. start returning to what Cline called its “post-Camp Fire normal,” with traffic increasing to 200-plus a day.
“It actually makes our staff feel reassured: ‘Oh, our people are back,’” she said. “We don’t want people to have to come to the ER, but we knew they were coming before.”
Enloe has resumed elective procedures, and last week the hospital announced it would be replacing tents in the separate COVID-19 triage area with a climate-controlled modular building.
“The most important concern is [if] people delay care that they really need because they’re concerned about either getting a COVID infection in a hospital or a clinic, or because they’re trying to be good citizens and stay away,” Wiltermood said. “I can tell you for an absolute fact that we have lost far more people due to delays in care than we have due to COVID.”
Should Enloe need to ramp up for a full-on surge, Wiltermood said the medical center could again postpone elective surgeries, reallocate space—in the hospital’s intensive care units and south wing (for around 75 additional beds with ventilators), plus certain clinics—and, within 48 hours, convert the rehab center into a field hospital again.
Space isn’t necessarily the key factor, though, at Enloe or other facilities. Wiltermood listed adequate supplies, particularly protective equipment; sufficient testing for COVID; and, foremost, keeping staff healthy.
“The initial plan for all the mitigation efforts was to flatten the curve, to prevent everyone from getting sick and overwhelming our health-care system at one time,” York said. “It’s extremely necessary that everyone continues to be vigilant and participate in all of the [preventative] activities we have been doing.”


Be the first to comment