
As coronavirus vaccines have grown more widely available to the general public in recent months, health officers across the country set their sites on achieving herd immunity: developing collective protection against COVID-19. Over time, they’ve differed wildly on the extent of vaccination needed to reach this point—anywhere from 60 to 90 percent—though most projections center on 70 to 75 percent of the population.
Butte County Public Health supported that assessment—and, scientifically speaking, the department still does. But county officials, like colleagues nationwide, no longer hold fast to herd immunity as a fixed goal. Debate swirls as to whether that level is attainable or even applicable in this pandemic.
Just yesterday (May 13), U.S. Surgeon General Vivek Murthy told attendees at the Future is Everything Festival that herd immunity “is not a switch you turn on and off.” COVID-19 presents a moving target.
Preeminently important, from the perspective of public health officials and many others, is keeping the most at-risk people—seniors and those with chronic conditions—from contracting coronavirus. If true herd immunity isn’t achieved, the thought is that if at least the most vulnerable are vaccinated at a high rate—as of today (May 14), 72.1 percent of adults 65 and over are fully vaccinated—the level of hospitalizations and deaths will be minimized, and that goes hand in hand with reestablishing normalcy.
A huge factor impeding herd immunity is vaccine resistance. Even though willingness has increased since the rollout, 25 percent of Americans still say they won’t get vaccinated. A vocal segment of this population spreads social media messages that contradict medical findings backed by local and state health departments, the U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization.
As demand for vaccinations among adults has slowed, Butte County Public Health has conducted outreach efforts—including recently surveying residents who hesitate to get vaccinated.
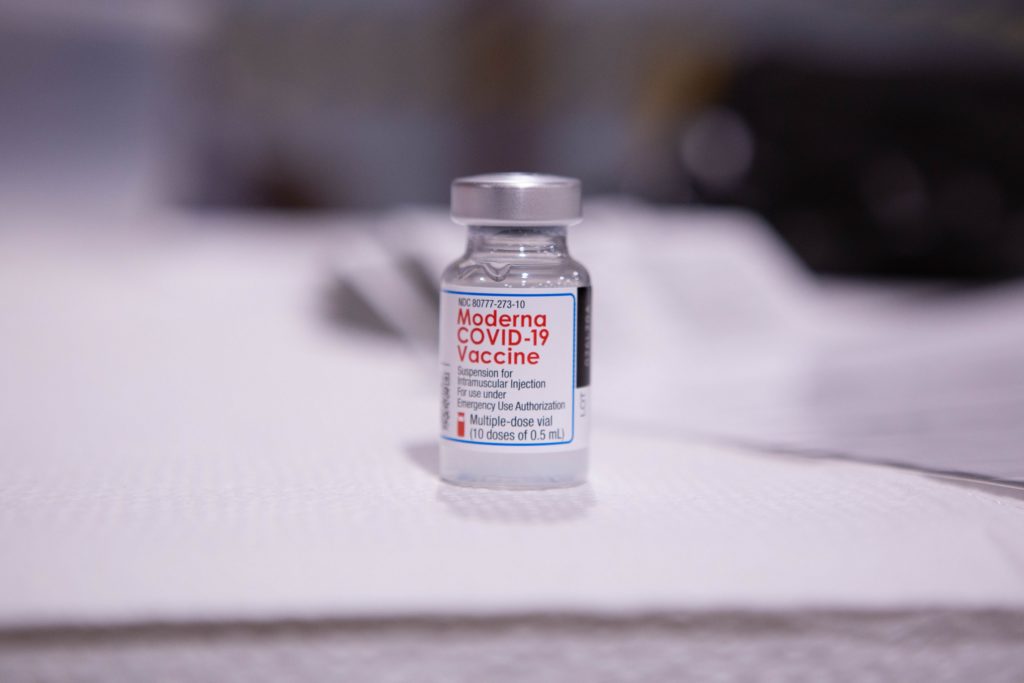
Meanwhile, opportunities for youth have just expanded. Monday (May 10), the U.S. Food and Drug Administration (FDA) added adolescents between 12 and 15 to the emergency use authorization for the Pfizer vaccine, and yesterday afternoon, Butte County announced that this vaccine is now available to anyone 12 and older. The Moderna and Johnson & Johnson vaccines remain only for residents 18 and older. Clinical trials are underway for children under 12, with federal approval possible as early as this fall.
The county, with hospitals such as Enloe Medical Center, no longer operates large-scale vaccine clinics at Silver Dollar Fairgrounds and Meriam Park. Instead, vaccinations have shifted to facilities such as the Enloe Behavioral Health building and the Stonewall Alliance Center of Chico, in addition to being available at most major pharmacies. Over the past week, an average of 505 doses a day have been administered in the county—upping the total to 146,947 doses as of this afternoon.
Around 37 percent of Butte County residents have received one dose and 30 percent are fully vaccinated, as compared to 36 percent nationwide.
“We didn’t really set a specific goal of 70 to 75 percent, which is about what you’d want to call herd immunity,” Butte County Public Health Director Danette York told the CN&R by phone. “Our goal is more along the lines of getting as many people who qualify and want the vaccine vaccinated.

“I don’t think [herd immunity] is even possible, because of the percent of the population that can’t even get the vaccine at this point because they’re too young, and there’s always going to be the subset of the population that don’t want to get any vaccine.
“So, my opinion is it’s probably not reachable to try to get herd immunity, but that doesn’t mean we’re going to stop trying to convince people that getting the vaccine is a good idea.”
Science and optimism
Dr. Linda Lewis, Public Health’s epidemiologist, has a slightly different perspective. She says she “ha[s]n’t given up on herd immunity” entirely, viewing this community protection as a “path to normalcy.”
Much like Murthy, she clarified that “herd immunity is not like an all or nothing event. The closer we get to that event, the less disease we’re going to see, the fewer outbreaks, and the fewer lives we’re going to lose to this disease.”
Lewis estimated that children ineligible for the vaccine comprise 14 percent of the county’s population, and residents with health conditions precluding vaccination another 1 percent. That leaves a potential base of around 85 percent who could get vaccinated.
“I’m perhaps a bit more optimistic: I think we can still do it,” she said in a phone interview. “A big question mark in the equation, too, is how many people have natural immunity because of infection.” In other words, people who’ve contracted COVID-19. Public Health tracks those numbers—11,863 confirmed cases as of today, including 183 who have died—but does not add those to the vaccination numbers to ascertain herd immunity, Lewis said, because of potential overlap.
Public Health still is reviewing results from the survey on vaccine resistance, but Public Information Officer Lisa Almaguer relayed three of the most common reasons cited: safety, speed at which the vaccines was developed and side effects after the second shot. Lewis looks forward to a wider sample of perspectives. Public Health will utilize this feedback in its marketing and education efforts.
“At the very beginning, we made the determination in conjunction with our county administrative officer that we would follow the science,” York said of her department’s approach to COVID-19, including vaccines. “We would present and advocate for the best practices in what could be shown through the science.
“So, any time we get pushback from anyone who doesn’t believe that [the pandemic] is a real thing, or think that it shouldn’t have been an emergency or ended already, or protested, whatever, we just revert back to … ‘It’s been shown by the CDC and we have to follow the state guidelines.’ That’s what we’ve done.”
Public Health has worked to counter misconceptions (see CN&R article “Spreading innoculation”). In response to the public concerns, Lewis explained that pharmaceutical companies released vaccines quickly because they started production during the approval process rather than first waiting for the FDA’s emergency authorization. She also supported what Dr. James Moore told the CN&R in December when he received Butte County’s first dose (see “COVID vaccine arrives”), that the global spread of this coronavirus made for more patients simultaneously available for clinical trials compared to other illnesses, allowing for a much shorter than normal testing period.
As long as vaccines and emergency room beds remain available, whether or not people get innoculated, the county and state are hoping for a return to normalcy in one month when the economy fully reopens June 15 (see “‘Light at the end of the tunnel’”). Long-term, Lewis has a greater aspiration.
“Actually, my hope would be that we learn from this pandemic and we don’t go back to a ‘normal’ but we go back to a ‘better than before’—that we’re better about staying home when we’re sick; that we’re better about hand hygiene, covering coughs and sneezes; that we’re better about having good ventilation in schools and workplaces; that we’re better at worker health protection; and we’re even better about wearing a face covering if we’re under the weather and we need to go out in public.
“I don’t think COVID is going to go away,” Lewis continued, “[and] when COVID becomes more like flu, there will be another respiratory virus that comes around. It’s just a matter of when.”


I think it’s really alarming that our public health lead Danette York has an ambivalent attitude toward one of the most important public health measures we can pursue in this generation–vaccination against the deadliest virus in modern history. Instead, her goal is just to get it out to whomever is interested and call it a day. That’s totally unacceptable from a public health official. Where does this stop? Will we let restaurants allow infestations if they’ve tried their best to keep the back of house clean at the expense of customer health?
Thank you for your comment, Eric. It should be pointed out that York did not express ambivalence to the CN&R over vaccinations for COVID-19. The goal of the department she is in charge of, Public Health, is to make it available to everyone who wants it, as well as to employ outreach efforts to educate on the benefits to getting the vaccine. Reservations about whether herd immunity would be achieved were in response to circumstances out of the department’s control, including lack of vaccines available for a portion of the population (kids) and vaccine hesitancy on the part of a large segment of the public.
I agree with you Jason, but my biggest concern was the apparent lack of enthusiasm toward what I think of as core principles of public health: education and advocacy. I’d love to see more enthusiasm for helping the community understand the safety and efficacy of the vaccines (as we do for kids and parents today) and less “throw my arms up, it is what it is” resignation.
I hear your concern, Eric. I just want to make sure the CN&R hasn’t misrepresented the director. In my estimation, there’s probably no single person in Butte County who has done more to educate the public on COVID-19 than York.